What is the ‘skin test’?
The cornerstone of tuberculosis (TB) control in cattle and other species is the accurate detection and removal of animals infected with the bovine TB bacterium Mycobacterium bovis (M. bovis) before they can spread the disease to other animals.
The primary screening test for TB in cattle in the UK is the single intradermal comparative cervical tuberculin test (SICCT). This is commonly known as the tuberculin skin test, which is used throughout the world in its various formats to screen cattle, buffalo, bison, other animals and people for TB. It is the internationally accepted standard for detecting M. bovis infection in live animals.
How does it work?
TB in cattle is usually a chronic infection and clinical signs of the disease often take a long time to develop. Infected cattle can become infectious before they show any obvious signs or develop lesions in their internal organs. Therefore, rather than look for the bacterium itself, the skin test in cattle relies on measuring the immune response of the animal to injections of tuberculin. Tuberculin is a complex mix of proteins extracted from cultures of M. bovis grown in the laboratory and killed by heat.
The skin test is comparative as the animal’s immune response to injections of both bovine and avian (bird) tuberculin is measured and compared. By simultaneously injecting two types of tuberculin into the deep layers of the skin of the neck, the test can better distinguish between animals infected with M. bovis and animals previously exposed to or infected with other types of mycobacteria found in the environment which do not cause bovine TB.
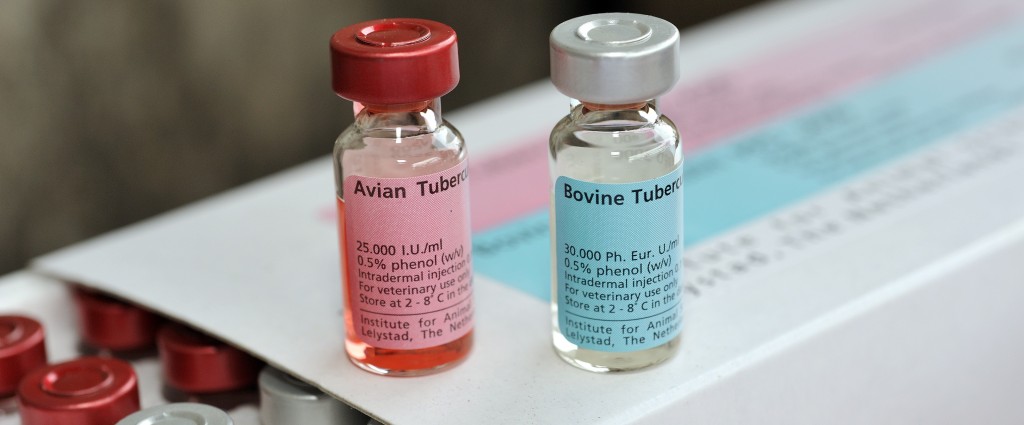
If an animal’s immune system has previously been ‘sensitised’ (primed) by infection with M. bovis or exposure to other mycobacteria, then the injection of tuberculin triggers an inflammatory response and a reaction (swelling or 'lump') develops at the injection site. The intensity of the reaction is greatest at 48-72 hours after injection, and subsides rapidly afterwards. Cattle that are infected with M. bovis tend to show a greater reaction to bovine tuberculin than avian tuberculin.

The size and nature of any reactions at the avian and bovine injection sites are measured and compared. Depending on the degree of reaction to the skin test and the interpretation of the test, the animal is classified as;
- Clear - negative result
- Fail - reactor or positive result
- Inconclusive reactor (IR) – the animal shows a reaction to bovine tuberculin greater than the avian, but not strong enough to be classified as a reactor. IRs must be isolated and re-tested after 60 days. Animals that have an inconclusive result at two consecutive skin tests are considered reactors
How is the skin test carried out?
Cattle keepers have a statutory responsibility to ensure that their animals can be safely TB tested. Guidance on safe handling of adult cattle is available from the Health & Safety Executive.
The tuberculin skin test is carried out on two days.
Injection of avian and bovine tuberculin.
- The ear tag number of the animal to be tested is reconciled with the list of animals on the test chart (or hand held device if applicable).
- The two injection sites are marked on the animal’s neck, usually by clipping the hair away with clippers or curved scissors.
- The skin thickness at each site is measured using callipers and the measurements are recorded against the animal.
- Avian tuberculin is then injected into the skin of the upper site and bovine tuberculin into the skin of the lower site.
Reading of the test 72 (+/- four) hours later.
- The animal’s ear tag number is confirmed against the testing record from day one.
- Each injection site is visually inspected and felt with the fingers for any reactions (swellings).
- Where there is any detectable reaction at either site, both sites are re-measured with callipers and the measurements and type of reaction recorded against the animal, along with the test result after interpretation.

Interpretation of the skin test
The skin test can be interpreted at either standard or severe interpretation. Standard interpretation is the default used for all routine surveillance testing, whilst severe interpretation is used in circumstances where TB is strongly suspected or confirmed e.g. for testing in TB breakdown herds.
Interpreting the test at severe interpretation involves lowering the cut-off point for an animal to be classified as a reactor. What this means in practice is that some animals considered inconclusive reactors at standard will become reactors at severe interpretation.
The severe interpretation used in England and Scotland is slightly different to the one used in Wales, where some clear animals at standard interpretation may become IRs at severe interpretation.
How accurate is the skin test?
No diagnostic test is perfectly accurate and there is a trade-off between sensitivity and specificity.
The probability that a test will correctly identify an infected animal as positive. The higher the sensitivity of the test, the lower the probability of incorrectly classifying an infected animal as uninfected (a false negative result).
The probability that a test will correctly identify an animal that is free from infection as negative. The higher the specificity, the lower the probability of incorrectly classifying an uninfected animal as infected (a false positive result).
The specificity of the skin test used in the UK is very high – approximately 99.98% at standard interpretation1. In practical terms, this means that you would expect approximately one false positive result for every 5,000 uninfected cattle tested using standard interpretation. This very high specificity gives us a high degree of confidence that the vast majority of the skin test reactors identified in high incidence areas of England and Wales are animals truly infected with TB, irrespective of whether or not lesions typical of the disease can be detected during post-mortem meat inspection in the slaughterhouse (see the next section on the predictive value of the test). Even in low incidence areas such as Scotland the majority of skin test reactors are likely to be truly infected with TB, irrespective of whether or not lesions typical of TB are found at slaughter.

However, the main limitation of the tuberculin skin test is its sensitivity. Studies have shown that skin test sensitivity in Great Britain lies between 52% and 100% with an average of about 80% sensitivity at standard interpretation¹ and slightly higher at severe interpretation. In practical terms this means that on average 20-25% of TB-infected cattle can be missed by one round of skin testing using standard interpretation.
The sensitivity and specificity of the skin test may be influenced by the stage and severity of the disease in each individual animal, exposure to other types of mycobacteria and a number of other factors.
The effect of using severe interpretation is to increase the sensitivity of the test over the standard interpretation. However, it is also important to realise that it lowers the specificity of the test (resulting in more false positive results) and this is why it is not used in routine surveillance testing.
Predictive value of the test
As well as the sensitivity and specificity, it is also important to consider the positive and negative predictive values of the skin test.
The probability that an animal with a positive test result is truly infected.
The probability that an animal with a negative test result is truly free from infection.
Positive and negative predictive values can be confused with sensitivity and specificity, but they are not the same. Sensitivity and specificity are purely characteristics of the diagnostic test itself, whereas positive and negative predictive values are a function of the sensitivity and specificity of the test and are also influenced by the level of disease in the population being tested.
Thinking about positive predictive value in the context of screening cattle for TB, we are essentially asking;
‘If a skin test discloses reactors, what is the probability that they are truly infected with M. bovis?’
If we skin test an Officially TB Free (OTF) herd located in the High Risk Area (HRA) and a reactor is disclosed, it is highly likely that the herd is truly infected with M. bovis as there is a high level of disease present in the area and we know that the probability of false positive results is very low. In this situation we would say that ‘the test has a high positive predictive value’ i.e. we are confident that the test is a strong indicator of infection.
It has been estimated that the positive predictive value of the skin test read at standard interpretation is approximately 92% in the HRA of England. This means that the vast majority of skin test reactors that are removed in that part of the country represent true infection with M. bovis, even when such animals show no visible lesions of TB at slaughter. The equivalent values for test reactors in the Edge Area and Low Risk Area (LRA) are marginally lower, but still quite high (approximately 88% and 77%, respectively).

A good herd test
The tuberculin skin test is often described as a good ‘herd test’, but a poor test for identifying individual infected animals. In fact any diagnostic test (not just the skin test) will have a greater chance of detecting infected groups of animals than infected animals tested in isolation.
Herd-level sensitivity (i.e. the probability that an infected herd is detected by a screening test) increases as the number of animals tested in the herd increases. This is still the case even if the level of disease in the herd is relatively low and the sensitivity of the test at individual animal level is less than perfect, since detection of one positive (reactor) animal is enough to declare the herd positive and infected with TB.
Why does the skin test miss infected animals?
There are many factors that can affect the sensitivity of the tuberculin skin test i.e. its ability to correctly identify an infected animal as positive. Potential reasons for missing infected animals (so called false negatives) are explained below.

The ‘pre-allergic’ period
Most animals take 3-6 weeks after infection with M. bovis to develop a full immune response that can be detected by the skin test. If an animal happens to be tested during this so called ‘pre-allergic’ (unreactive) period soon after infection, then it may not react to the skin test and hence will be missed.
Desensitisation
Desensitisation is the phenomenon whereby an animal’s skin reactivity to tuberculin is reduced for some time after the skin test. If another injection is administered too soon after the first without sufficient time for the animal’s immune system to recover, it can result in failure to react and therefore to identify infected cattle as reactors. This is why there is a minimum period of 60 days between skin tests, to prevent desensitisation. Repeated skin testing in chronically infected TB breakdown herds does not have a significant desensitising effect on cattle as long as the minimum 60 day interval between tests is observed.

Overwhelming infection with M. bovis
Cattle in the terminal stages of TB can have a depressed immune response that prevents them from reacting to the skin test – so called ‘anergy’. Despite having extensive lesions of TB in their internal organs, these anergic animals can still pass repeated skin tests and show no outward signs of ill health. Although rare, they present a significant risk of spreading TB as they can pass repeated skin tests undetected and spread infection within and between herds. Occasionally these anergic animals remain undetected until slaughter and extensive lesions typical of TB are discovered at post mortem examination (so called slaughterhouse cases). The supplementary interferon-gamma blood test can be useful in detecting some of these anergic animals as it is more sensitive than the skin test

Environmental mycobacteria
Mycobacteria other than M. bovis are found in the farm environment in soil, water, pasture, etc. and cattle are routinely exposed to them without harm. Even so, these mycobacteria can trigger false positive reactions to bovine tuberculin in the skin test. That is why in the UK we also use avian tuberculin alongside bovine tuberculin, since the cross-reactions (‘lumps’) triggered by these environmental mycobacteria tend to be larger at the avian than the bovine injection site during skin testing and this helps reduce the likelihood of false positive results. The flip side is that in herds that are also infected with M. bovis, truly infected animals can be missed as a large reaction at the avian injection site can mask the reaction at the bovine injection site and lead to the animal being incorrectly classified as negative.

Johne’s disease
Johnes disease is caused by the bacterium Mycobacterium avium subspecies paratuberculosis, which is closely related to M. bovis. Infection of cattle with this bacterium (or vaccination against Johne’s disease) can also cause cross reactivity with avian and bovine tuberculins and interfere with the interpretation of the tuberculin skin test in the same way as other environmental mycobacteria.

Suppression of the immune system
If the immune system of an animal is compromised for any reason, it is more susceptible to infection and may be less likely to react to the skin test (i.e. infected animals may be missed). Some of the more common reasons for depression of the immune system in cattle are listed below;
- Infection with viruses e.g. Bovine Viral Diarrhoea (BVD) or parasites such as liver fluke.
- Drug treatment (e.g. steroids).
- Suppression of the immune system during the early post-calving period.

Errors when carrying out the skin test
Although processes are in place for quality assurance of TB testers, tester error can still occur and this can lead to a reduction in the overall sensitivity of the test and the potential for missing infected animals. The main types of errors are;
- Improperly stored or out of date tuberculin.
- Too little bovine tuberculin injected in to the skin.
- Tuberculin not injected in to the skin correctly.
- Incorrect location of injection sites.
- Injection of bovine tuberculin in the avian injection site and vice versa.
- Reading the test too early or too late.
- Errors in recording skin measurements
- Errors in identifying reactor animals.
Who checks that TB testing is carried out correctly?
TB testing and other official veterinarian (OV) work in England and Wales is undertaken by Veterinary Delivery Partners, who are responsible for allocating local vets and ensuring that TB testing is carried out to a high standard. In Scotland, TB testing is delivered through OV practices.
APHA carries out risk-based audits of OVs carrying out skin testing to check that it is being carried out correctly in line with agreed procedures. Further details are available on the APHA website.
Synchronisation of TB skin testing in England

Cattle herds located at two or more holdings may have their TB skin testing synchronised by APHA. This means that all eligible cattle at the separate locations are skin tested within the same testing window.
Examples of situations where TB skin testing is synchronised between cattle herds are described below. This applies to routine and enhanced surveillance testing, and TB breakdown testing. Please note that this is not an exhaustive list and keepers are advised to contact APHA to discuss their individual circumstances.
- In most cases, APHA synchronises TB skin testing between cattle herds located at a permanent CPH (pCPH) and one or more temporary CPHs (tCPH).

- Two or more cattle herds kept at separate holdings (different pCPH numbers) under the same ownership may have their TB skin testing synchronised on request subject to assessment by APHA.
- Two or more cattle herds kept at separate holdings (different pCPH numbers) but under different ownership may have their TB skin testing synchronised on request subject to assessment by APHA. For example, family members or neighbours with separate cattle herds may wish to synchronise their herds’ routine TB testing so that they can test the animals within the same testing window (each herd at their own holding) and share mobile handling facilities and/or labour.
Please note that two or more cattle herds (different pCPH numbers) kept and run together at the same location is no longer allowed. For more information on registering temporary land, see the guidance on GOV.UK.
TB testing regimes across different bTB risk areas in England
There are situations where a keeper has cattle herds located in more than one bTB risk area. The general principles for setting the frequency of surveillance TB testing in these situations are outlined below, however you are advised to contact APHA to discuss your individual circumstances.
- Cattle located at a tCPH in the Low Risk Area (LRA) associated to a pCPH in the High Risk Area (HRA) or Edge Area are TB tested at the frequency of cattle located at the pCPH i.e. the more frequent of the testing intervals.
- Cattle located at a tCPH in the HRA or Edge Area associated to a pCPH in the LRA are TB tested at the frequency of the area in which the tCPH lies i.e. six-monthly or annual testing. The pCPH retains its own testing frequency because pre- and post-movement testing requirements apply, however APHA may review this based on the volume, regularity, frequency, and nature of cattle movements into the LRA from tCPHs in the HRA and Edge Area.
- Annual surveillance testing applies to any tCPH in the LRA associated to a pCPH in the LRA which is subject to permanent or temporary annual (or more frequent) testing. Pre-movement testing also applies unless there are any current exemptions.
- When land registered under a pCPH straddles two different TB testing areas, surveillance TB testing of the herd defaults to the more frequent testing regime.
Non Visible Lesion (NVL) reactors
In the UK, approximately 40% of all skin test reactors show visible lesions typical of TB at post mortem meat inspection and/or isolation of M. bovis on culture. It is important to recognise that this is due to the relatively insensitive methods of confirming infection with M. bovis at slaughter, and not a failure of the skin test. The specificity of the skin test is approximately 99.98% and therefore animals identified as positive are highly likely to be truly infected with M. bovis, regardless of their post mortem or culture result.
Post mortem examinations (particularly when carried out in a commercial slaughterhouse setting) and culture are far less sensitive than the tuberculin skin test and interferon-gamma blood test.
A skin test reactor that showed no visible lesions at post mortem meat inspection can occur for the following reasons;
- The animal was in the early stages of infection with M. bovis when TB lesions are too small or infrequent to be observed by the naked eye
- The animal had visible lesions at post mortem inspection, but they were missed during a relatively quick post-mortem inspection at the slaughterhouse.
Summary
- The main limitation of the tuberculin skin test is its sensitivity. On average 20-25% of TB-infected cattle can be missed by one round of skin testing using standard interpretation. In certain situations the sensitivity of the skin test is increased by using severe interpretation and thereby lowering the cut off point for a positive result. The interferon-gamma blood test is also used to supplement the skin test in certain scenarios to increase the sensitivity of TB testing.
- The skin test is highly specific, which means that we can be confident that the vast majority of skin test reactors identified in the high incidence areas of England and Wales are truly infected with TB, irrespective of whether or not lesions typical of TB are found at slaughter. Even in low incidence areas, such as Scotland, the majority of skin test reactors are likely to be truly infected with TB, again irrespective of whether or not lesions typical of TB are found at slaughter.
- False negatives (TB-infected animals missed by the skin test) can occur for a variety of different reasons including environmental mycobacteria, Johnes disease/vaccination, suppression of the animal’s immune system for any reason, cattle in the terminal stages of TB infection and errors when carrying out the skin test.

Useful resources
- More information about TB testing of cattle on GOV.UK
- Tuberculin skin test factsheet
- Interpretation of the skin test in Great Britain
- Veterinary Delivery Partners