What is TB and how is it transmitted?
Tuberculosis (TB) is a chronic, primarily respiratory infectious disease of mammals caused by a group of closely related bacteria known as the Mycobacterium tuberculosis (MTB) complex. This group includes:
- M. bovis – responsible for TB in cattle (bovine TB) and other mammals, including occasionally people. Cattle are the natural host of M. bovis, but nearly all warm-blooded animals, including goats, deer, pigs, camelids, sheep, cats and badgers are susceptible to the infection. This broad range of animal hosts complicates the eradication of bovine TB.
- M. tuberculosis – the primary cause of TB in people, which rarely causes disease in animals.
This guidance is mainly concerned with TB caused by M. bovis and all further references to ‘TB’ denote the disease resulting from infection with M. bovis.
Sheep are susceptible to M. bovis and can develop lesions and clinical signs of TB. However, they are regarded as spillover hosts. In other words, sheep can become infected only when the challenge level is relatively high, and they do not usually sustain the infection within their own populations in the absence of infected cattle or a wildlife reservoir. TB incidents in sheep flocks in Great Britain (GB) are infrequent. The infection can spread either directly (animal to animal) or indirectly via materials contaminated with the secretions or excretions of infectious animals. This can include contact with:
- infected cattle and other domestic animals (e.g. sheep, goats, camelids)
- wildlife reservoirs of infection
- contaminated, pasture, equipment, feedstuffs, water and slurry

Infection with M. bovis is also a zoonosis, meaning that it can be naturally transmitted from vertebrate animals to humans, although the risk of sheep-to-human transmission of M. bovis is considered to be very low, with no cases ever documented in GB so far. A potential route of transmission to humans is through the consumption of unpasteurised (raw) milk and dairy products from TB-infected milking ewes.
A very small number of laboratory-confirmed incidents of TB are reported every year in sheep flocks in GB. Official statistics relating to TB in sheep (and other non-bovine livestock species) in GB are published on GOV.UK.
Signs of TB in sheep
There is no routine surveillance TB testing of sheep in GB. M. bovis infection is usually chronic (slowly-progressing), insidious and, because its clinical signs are not specific, it is difficult to diagnose in sheep by clinical examination alone. Most cases of TB in sheep are usually identified at post-mortem meat inspection in the slaughterhouse, or through post-mortem examination of carcases submitted to a veterinary diagnostic laboratory.
Actions when M. bovis is suspected in sheep

TB in sheep is a notifiable disease in GB, which means there is a legal obligation to report suspicion of disease. In England and Scotland, if, following a clinical or post-mortem inspection or examination, the animal or carcase is suspected to be infected with TB, the Animal and Plant Health Agency (APHA) must be notified without delay by the person who has raised the suspicion. In Wales, TB is only notifiable in a sheep carcase or following identification of M. bovis by laboratory examination of samples taken from the animal. APHA will then place movement restrictions on the whole flock, or part of the flock, by serving a restriction notice. Additional movement restrictions may also be applied, in Wales, on other TB susceptible species on the holding. These restrictions will remain in place until APHA is satisfied that the suspicion of TB is ruled out or that all TB infected animals have been identified and removed
PCR testing of suspect TB lesions in a sheep carcase
APHA routinely uses Polymerase Chain Reaction (PCR) testing on tissue samples collected at post-mortem inspection as the primary test to confirm or negate suspicion of M. bovis infection in sheep carcases.
The PCR test reduces the time taken by the APHA laboratory to confirm whether M. bovis is present in tissue samples taken from carcases at post-mortem inspection. This means that in certain situations (i.e. slaughterhouse cases), if the PCR test results are negative, and check testing of the flock has been completed where required, APHA can lift flock movement restrictions sooner than when the previous laboratory protocols based on bacteriological culture were in use (which typically took 6-22 weeks to complete). If the PCR test results are positive, APHA can inform the keeper and their private vet quickly, so that further action can be taken as soon as possible to control TB in the affected flock.
Actions when M. bovis is confirmed in a sheep flock
APHA will undertake a veterinary risk assessment when M. bovis infection has been confirmed by PCR testing (or bacteriological culture) in a sheep flock to determine the appropriate TB testing protocol and other actions taken by APHA. These will include movement restrictions and likely a combination of slaughterhouse investigations, tuberculin skin testing and tracings. Two consecutive skin tests of the flock, completed at 60–day intervals, with negative results are required to lift restrictions. Skin testing in this scenario is government-funded.

Skin testing of sheep
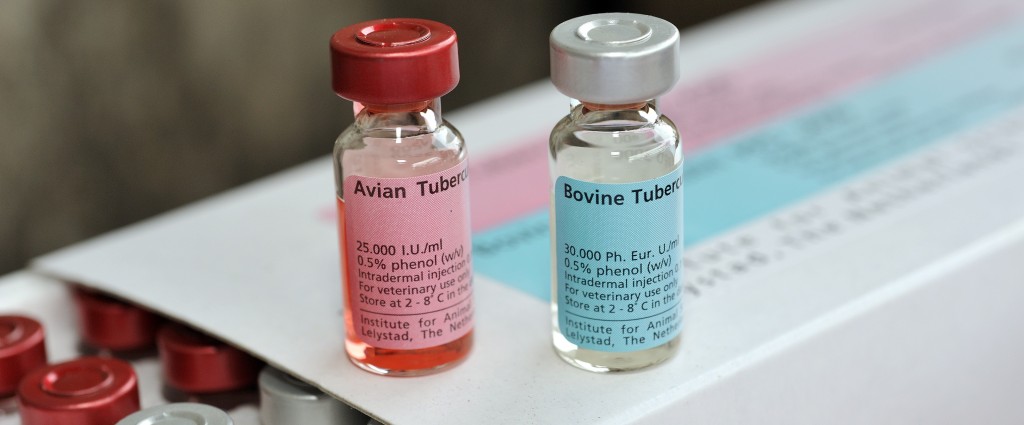
The tuberculin skin test is commonly used for TB screening of live sheep. This involves a comparative test, injecting a small amount of avian and bovine tuberculin (a sterile, purified mixture of proteins extracted from cultures of M. bovis) into the deep layer of the skin in the middle of each side of the neck, (or alternatively in the groin area). The skin is first clipped and the thickness of the skin fold measured in millimetres using special callipers before the tuberculin is injected. After 72 ± 4 hours, the vet returns and re-measures the skin at the site of the injections to determine if the animal is classified as a reactor, inconclusive reactor or negative (pass). The standard operating procedure for official veterinarians carrying out tuberculin skin testing of sheep can be found on the APHA Vet Gateway.
Where skin testing is considered impractical or inappropriate, alternative methods of surveillance of the TB status of a flock may be considered, such as surveillance through post–mortem examination at a slaughterhouse. However, this will most likely significantly extend the time that the flock is under movement restrictions.
Sheep co-located with cattle on TB breakdown premises

When cattle on a farm are under movement restrictions for a TB breakdown and APHA considers that there is a risk of infection spreading from cattle/badgers to other livestock on the same premises, a notice may also be served to contain other farm livestock, including sheep, into a defined part of the premises, away from the cattle and to prevent the movement of these animals to other holdings.
APHA will not normally restrict and TB test sheep that are co-located with (or contiguous to) a restricted cattle herd unless justified by a veterinary risk assessment, e.g. when sheep have been housed in close contact with infected cattle in a building with a shared airspace for a prolonged period.
Tracings
APHA will consider, on a case-by-case basis, whether breeding sheep that may have been moved out of an infected flock to another flock before the application of TB movement restrictions may need to be traced and tested at APHA’s expense.
Source (back) tracing investigations and skin check testing of the flock(s) of origin of purchased TB-infected sheep may also be undertaken.
Removal of skin test reactors
In the event of positive skin test results, APHA will:
- arrange and meet the cost of haulage and slaughter of the reactors and any direct contacts (DCs)
- arrange and meet the cost of post mortem examination (PME) of the reactors and any DCs and laboratory testing (PCR or culture) of samples where appropriate
- allow private slaughter if the owner wishes (in this case the owner will meet the costs of haulage and slaughter)
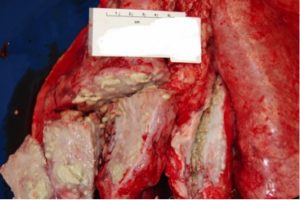
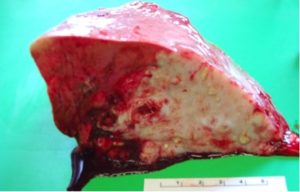
Post-mortem images of TB in sheep
TB lesions in sheep are primarily reported in the lungs and thoracic lymph nodes. Lesions are cream, yellow or green in colour and may be calcified (gritty).
Compensation for compulsorily slaughtered sheep
There is legal provision for the government to pay compensation to keepers for sheep that are identified as reactors or DCs and require compulsory slaughter. Compensation rates are determined under the relevant domestic legislation for each country:
- In England, the Tuberculosis (Non-bovine animals) Slaughter and Compensation (England) Order 2017
- In Wales, compensation rates are determined by more general powers under the Animal Health Act 1981
- In Scotland, the Tuberculosis in Specified Animals (Scotland) Order 2015
In England and Scotland, statutory compensation payments for sheep which are compulsorily slaughtered by APHA for TB control reasons are as follows:
- £80 for a lamb aged 1 year old or younger
- £130 for a breeding ewe over 1 year old
- £350 for a breeding ram over 1 year old
In Wales, compensation for sheep slaughtered due to TB is paid in accordance with the slaughter value as agreed with APHA and supported by evidence from current published slaughter values for sheep.
Sheep owners in GB can arrange for the private slaughter of the animals if they wish. In such cases, they will forgo the statutory compensation payments, but will retain any salvage value of the carcases. Additionally, APHA will not accept responsibility if the carcase is condemned and will not pay compensation or any privately arranged haulage retrospectively.
Free biosecurity advice for sheep keepers in England
The TB Advisory Service (TBAS) provides free, bespoke advice about practical, cost-effective measures to build herd/flock resilience to TB through on-farm advice visits and telephone advice. Keepers of farmed non-bovine animals across England are eligible for free advice from TBAS.
Sheep keepers can request a free one-to-one visit with an experienced veterinary advisor, who will provide bespoke recommendations to reduce the risk of TB infection for flocks. Contact TBAS via email at info@tbas.org.uk or over the phone on 01306 779410 to book your free advice visit.


Useful resources
- Defra guidance on managing TB in non-bovine animals, including movement restrictions and compensation
- Guidance on managing TB in non-bovine animals in Wales and Scotland
- Great Britain small ruminant quarterly report (disease surveillance and emerging threats) July to September 2021 (publishing.service.gov.uk) page 5-8 of the report show background on TB in sheep and case studies
- Defra routinely publish statistics on cases of TB in non-bovine species in Great Britain based on information collated by APHA